Newborns have an immature immune system and are vulnerable to infectious agents. The immune system begins to mature with appropriate interaction with antigens and is enhanced by the changing microflora of the gut throughout adolescence and adulthood.
Of course, aging affects all the systems of the body, and the immune system is no exception. The changes in immune system function that result from aging have been well characterized and are known as immunosenescence.11
In essence,
this can be described as a loss of immune “reserve” on the one hand and a loss of immune discretion on the other. Meaning that while most measurable features of the immune system decline over time, some may actually increase, such as autoantibody
production or inflammatory upregulation. These changes create increased susceptibility to infectious diseases, poor immunization response, and an increased risk for cancer and several autoimmune conditions. Likewise, the increased level of inflammation,
sometimes called “inflammaging,” mediates a number of well-known chronic diseases.
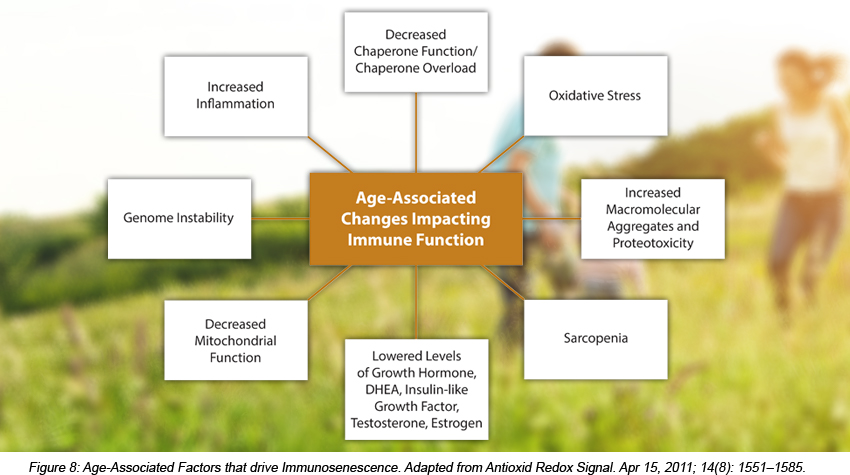
Aging cells of all kinds are burdened with a number of functional disruptions: decreased mitochondrial function, increased DNA instability, higher
amounts of unquenched reactive oxygen species (ROS), inefficient protein folding and a build-up of cellular toxins (See Figures 8 and 9).
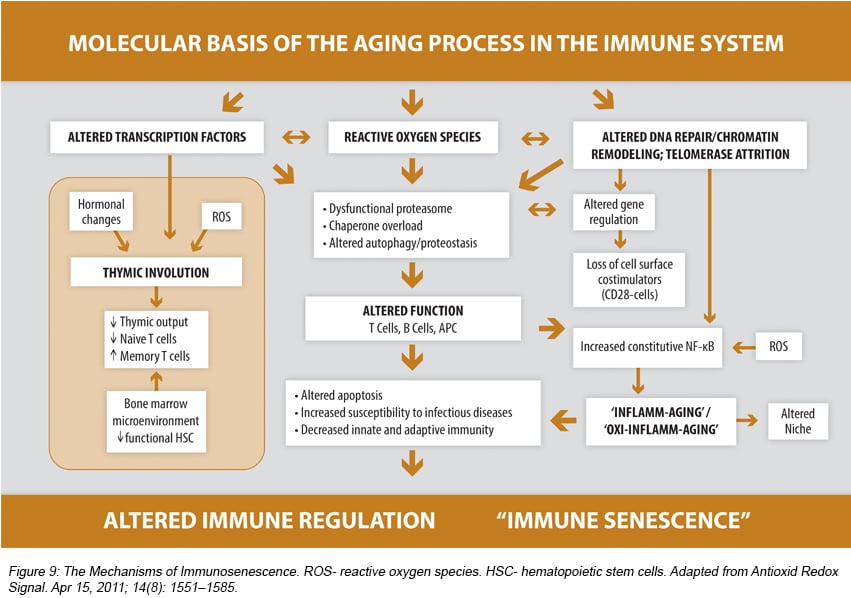
Since the lifespan of many immune cells is quite long, especially B and T cells, these disruptions can be cumulative.12 Furthermore, the result of fewer memory B and T cells combined with diminished bone marrow and thymus function (to
provide na�ve lymphocytes) adds to the loss of adaptive immune functions.13,14 After decades of dysfunction and cell apoptosis, the immune system is depleted in specificity, diversity and appropriate regulatory control.
While experienced by everyone, the consequence and impact of immunosenescence is highly dependent on the interplay of genetics, epigenetics, environmental factors and lifestyle-related signals from diet, physical activity, sleep and stress management.
The relative ratio of cortisol to DHEA levels (typically higher as one ages), growth hormone expression, thyroid function and antioxidant reserve capacity are critical in determining the rate and severity of age-related immune dysfunction.
Healthy lifestyle choices over many decades will strengthen and build the metabolic reserve that allows immune cells and organs to function well into the eighth and ninth decades of life. Supporting immune function in the aging patient requires
understanding, assessing and supporting each of these important parameters.
Excerpted from Supporting Immune Function: A Lifestyle and Nutrient Approach by Thomas G. Guilliams, Ph.D.
References:
- 11 Ponnappan S, Ponnappan U. Aging and immune function: molecular mechanisms to interventions. Antioxid Redox Signal. 2011 Apr 15;14(8):1551-85.
- 12 Fulop T, Le Page A, Fortin C, Witkowski JM, Dupuis G, Larbi A. Cellular signaling in the aging immune system. Curr Opin Immunol. 2014 Jun 13;29C:105-111.
- 13 Pritz T, Weinberger B, Grubeck-Loebenstein B. The aging bone marrow and its impact on immune responses in old age. Immunol Lett. 2014 Jul 8. pii: S0165-2478(14)00129-1.
- 14 Chinn IK, Blackburn CC, Manley NR, Sempowski GD. Changes in primary lymphoid organs with aging. Semin Immunol. 2012 Oct;24(5):309-20
 | About Thomas G. Guilliams Ph.D. Dr. Guilliams earned his doctorate from the Medical College of Wisconsin (Milwaukee) where he studied molecular immunology in the Microbiology Department. Since 1996, he has spent his time studying the mechanisms and actions of natural-based therapies, and is an expert in the therapeutic uses of nutritional supplements. As the Vice President of Scientific Affairs for Ortho Molecular Products, he has developed a wide array of products and programs which allow clinicians to use nutritional supplements and lifestyle interventions as safe, evidence-based and effective tools for a variety of patients. Tom teaches at the University of Wisconsin-School of Pharmacy, where he holds an appointment as a Clinical Instructor; at the University of Minnesota School of Pharmacy and is a faculty member of the Fellowship in Anti-aging Regenerative and Functional Medicine. He lives outside of Stevens Point, Wisconsin with his wife and children. | |
 |  |  |
| Learn More | Learn More | Learn More |