“I’ve got a gut feeling about this”
While we have certainly heard that appetite and digestion are controlled by the enteric nervous system (also known as “the master control panel
in your gut”), who would’ve thought that the gut might also control your emotions and mood? It’s no wonder the old sayings, like “I’ve got a gut feeling about this“, “That movie was gut-wrenching“,
or “Come on, gut it out!” ring so true. In fact I’d venture to say when we are trusting our intuition we associate it with having a “gut feeling” about something.
From the research it is now clear
that gut microbes have an affect on inflammation, pain, eating behaviors, food cravings, mood and other seemingly unrelated symptoms, such as depression or uncontrolled anxiety. In addition, it is common for depression and anxiety to co-exist
with disorders such as IBS (irritable bowel disorder).
It goes both ways…
Yes, it’s true! Did you know the gut-brain axis provides a way of communicating both directions using
signals, such as neurotransmitters, hormones and cytokines? This means that your gut bugs actually talk to your brain to influence emotions. Equally important the emotions you feel and neurotransmitters produced by the brain have a profound
effect on the gut as well. We know that dysfunction in this communication between gut and brain can lead to various diseases, including depression and anxiety. Who knew that the composition of your gut microbes could play such a great
role in your mood? The next time you get angry at your spouse or are overcome with sadness making you want to curl up in bed you can simply say, “Don’t blame me…It’s my gut microbes’s fault!” and you
may be right on target!
The human gut is populated by more than 100 trillion microbes, which means there is more bugs in your gut than cells in your body. And the genetic material contained by microbes in your gut is 150X that
of the genetic material from human origin. Most experts agree we have more than 1000 different species in our gut and over 7000 different strains. We know that as we are exposed to stress, chemicals, antibiotics, and toxins, the diversity
of the microbiome decreases and we know that the less diverse or microbiome, the more susceptible we are to illness and disease.
A baby’s colonization of the gut first occurs at birth with vaginal exposure to the mother’s microflora.
Did you know that c-section baby’s have gut microbes more akin to skin flora than gut flora after birth? And some studies show that throughout the entirety of life, they may never regain the normal diversity of vaginally delivered infants.
These are just a few of the functions of these bugs residing in your gut:
- Development of your immune system function
- Assisting with bowel movements and gut motility
- Maintaining intestinal cell barrier integrity (keeping the the good stuff in and the bad stuff out)
- Aiding in digestion and absorption of specific vitamins and minerals
- Controlling fat absorption and distribution
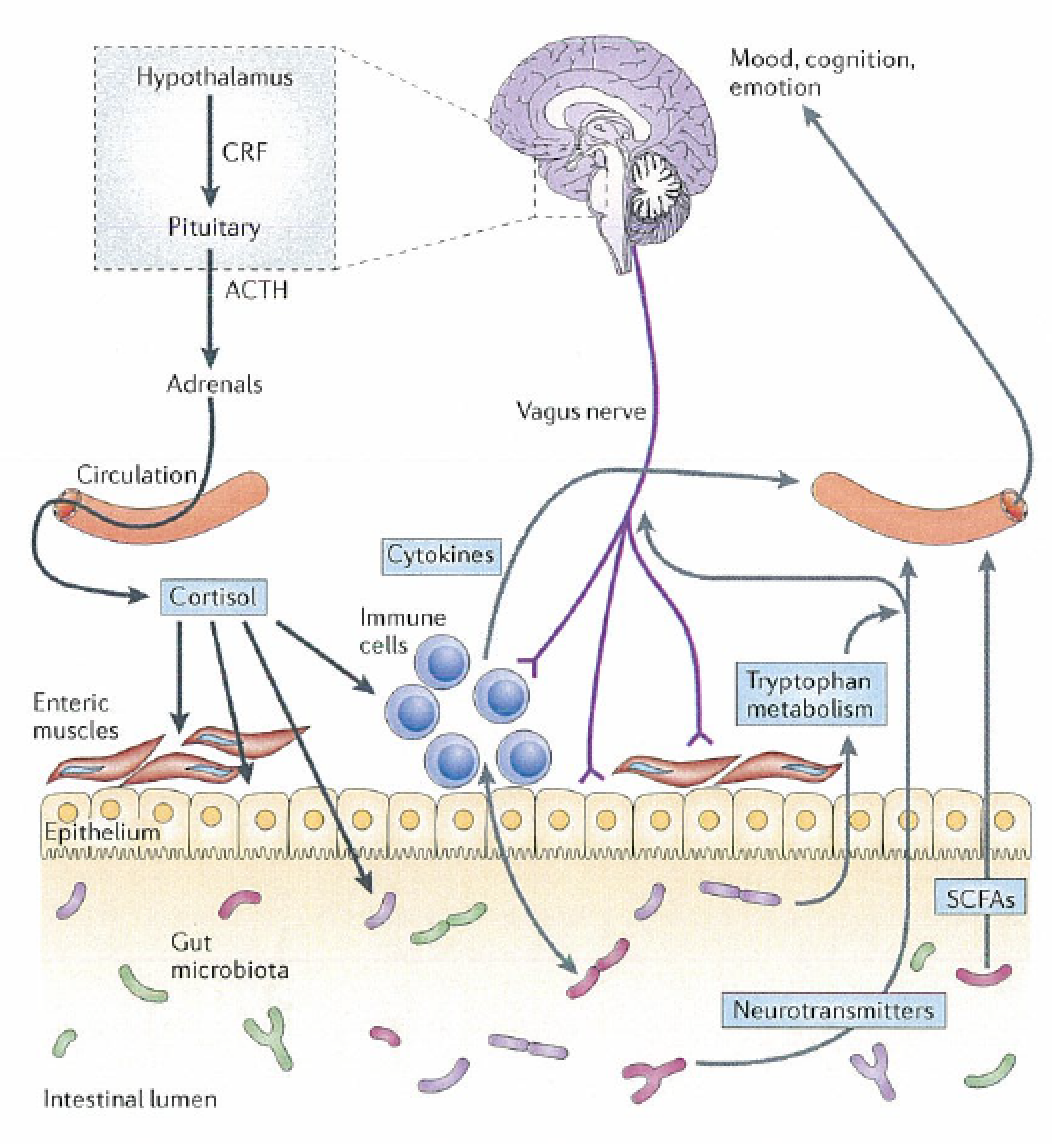
Microbes and Stress
What is increasingly clear is that there is bi-directional communication between our gut microbes influencing the central nervous system and brain… and the reverse; communication
between our brain influencing microbial composition. Did you know that stress affects the gut microbes, too?
These are the top 3 ways that chronic stress affects the gut:
- Increases the levels of inflammatory cytokines (IL-6, TNF-alpha) which can changes gut microbe populations.
- Increases permeability of the gut lining, which is linked to many autoimmune diseases (Hashimoto’s thyroiditis, lupus, rheumatoid arthritis, multiple sclerosis and many others).
- Allows bacteria to cross over into the bloodstream where the bacterial coating (LPS) can trigger an intense inflammatory response in the body.
So how do the gut microbes contribute to anxiety and depression?
Here are some of the mechanisms by which the gut microbes influence the brain and emotions:
- Altered microbial composition: Both probiotic (“good guys”) administration and harmful infectious bacteria (“bad guys”) have both shown to have an effect on the brain and emotions. One study showed supplementation with probiotics decreased anxiety.
- Immune Activation: Bacteria in the gut have been shown to activate the immune system and increase production of harmful pro-inflammatory cytokines. There are many studies showing a link between increase in certain cytokines and depression (see below if you want to read more)
- Vagus nerve: This is one of the main controls of the parasympathetic system that calms our fight or flight response and allows our body to relax and feel calm. Activation of the vagus nerve and release of acetyl-choline has been shown to have a profoundly calming and anti-inflammatory effect on the body. Most of the effects of gut microbes on the brain and body have been shown to be dependent on vagal nerve activation.
- Tryptophan metabolism: Tryptophan is an extremely important amino acid and the raw material needed to make serotonin (think “the happy neurotransmitter”) by the body. There is a pathway, called the kynurinine pathway that involves metabolism of tryptophan and accounts for nearly 95% of the stores of tryptophan in the body. In the case of pathogenic microbial infections in the gut (bacteria, yeast, or parasites) this pathway may be activated and “steal” from your body’s tryptophan stores. This leads to depletion of serotonin stores and may result in insomnia and depression.
- Microbial metabolites: Bacteria in the gut help produce bile acids and short chain fatty acids (SCFAs) which are essential for human physical and mental health.
- Neurometabolites: Crazy but true… bacteria have the ability to produce many neurotransmitters and metabolites that have direct action on brain and thought. Did you know studies show microbes can even influence your food cravings?!
- Bacterial cell wall sugars: Perhaps most fascinating of all, the outer coatings of bacteria contain sugar molecules that can directly signal immune and hormonal systems into action. This is the mechanism thought to be responsible for the healthy effects of probiotics on the gut and brain.
The bottom line is there is a growing body of evidence that suggests gut microbes play a large role in regulation in behavior and brain chemistry and are relevant to development of depression and anxiety.
So perhaps the best antidepressant
is a healthy whole food diet and a high potency probiotic to fuel a healthy gut microbiome!
See original blog post here
 | About Jill Carnahan, MD | |